Imagine a future in which treatment goals we once thought unattainable could be reached. GSK, along with global specialists and patient organisations, is aiming to achieve just that by applying years of expertise in respiratory disease, and a deep understanding of the immune system, to develop solutions that help as many people with asthma as possible achieve clinical remission.
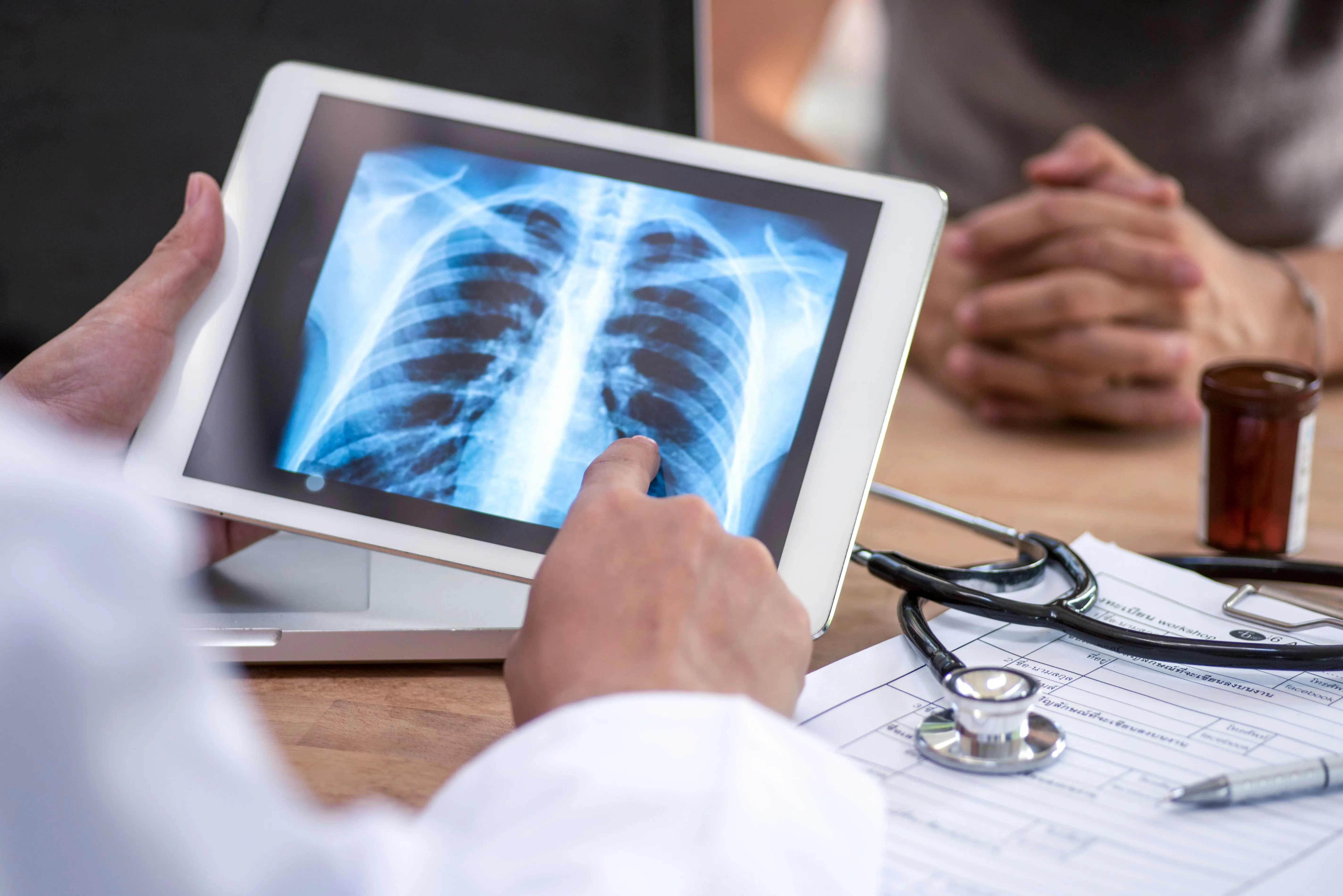
Asthma – a chronic lung disease caused by inflammation and muscle-tightening around the airways – affects more than 300 million people worldwide.
People with severe asthma can face years of frustrating trial and error approaches to treatment options before they receive a specific diagnosis of their type of asthma and receive the most appropriate management plan and therapy for them. Alongside the ongoing damage caused to a patient’s lungs due to avoidable attacks – known as exacerbations – this arduous process can also impact their mental health, work and social life.
Shelby Gorman, a GSK employee, knows all too well the negative impact of severe asthma on a child’s life. Shelby’s daughter, Joelle, has recently turned 18. She was diagnosed with severe asthma aged 14.
“The doctor said to us, ‘When was the last time you had a day when you felt good all day?’,” Shelby says.
“My daughter couldn’t remember. She could not remember one day when she felt well ever, in her life. I think it’s so important for doctors to understand that, beyond the condition, how bad severe asthma can make people feel.”
The concept of clinical remission as a treatment goal has only been applied to asthma in recent years. Thankfully, scientists and doctors have a far greater understanding of the different biological causes of asthma and the importance of an individualised approach today. They now know that not all asthma is the same, and that the underlying drivers of symptoms and exacerbations vary from person to person.
Two key goals of clinical remission are for people with asthma to be free from exacerbations or the need for oral corticosteroids (OCS) - steroid hormones that are effective at treating uncontrolled asthma, but can end up damaging healthy parts of the body.
Geoffrey Chupp, Professor of Medicine and director at Yale Center for Asthma and Airways Disease, says: “I think it’s really exciting that we’re talking about ‘how’ to achieve remission in patients with asthma as opposed to ‘if’ we can, and so I think we’re going to start to recognise that it could be possible to achieve remission in some patients.”
What is clinical remission in asthma?
The full definition of clinical remission in asthma is the absence of exacerbations for 12 months, the absence of symptoms, no use of OCS for at least 12 months and optimised or stabilised lung function.
Experts also include the optimisation of lung function as a fourth parameter. However, this may be difficult to achieve if there has been a delay in medical intervention, or if irreversible lung damage has accumulated after each exacerbation.
For people with asthma, clinical remission can mean not having to experience frightening exacerbations, hospitalisations, and the side effects of OCS, which can include weight gain, anxiety and sleep disturbances. Long-term use is also associated with an increased risk of diabetes, cataracts and osteoporosis. Some patients have additionally reported that the emotional burden of severe asthma has reduced and that they can enjoy daily activities without debilitating symptoms.
After many years of trying multiple different medications, and frequently being hospitalised due to exacerbations, Shelby’s daughter received a more accurate diagnosis of her asthma. This identified the underlying biological cause of her asthma and led to her starting appropriate targeted treatment. For the first time she was able to live her life with renewed energy and vigour.
Joelle hasn’t needed her rescue inhaler for over a year, has not had any respiratory infections and no longer needs to take daily antihistamines.
“I noticed the changes and said to my daughter, ‘Oh my gosh, you just got up the stairs, and you’re not out of breath,’” Shelby says.
“She would be like, ‘Oh yeah, oh my gosh!’ We would go for a little walk with the dog, and she would say, ‘No, I can do another lap, let’s do another lap, I can do it.’ And then we realised it had been months since she required any intervention of a nebuliser. Then we realised she was sleeping through the night.”
Remission in asthma is an incredible achievement. However, it is not a cure. With the right treatment as early in their treatment journey as possible, some patients will achieve remission. Although free from exacerbations and the need for OCS, the right medication or combination of medicines could maintain this over time.
Some patients may still need to use their rescue inhalers occasionally and, due to the nature of severe forms of asthma, even once remission has been achieved, there’s a chance that a patient’s condition could still deteriorate over time.
Preventing deterioration by reducing the risk of common infections with vaccines, or timely interventions with appropriate, evidence-based treatments, could stave off the disease progression of asthma and the lung damage it can cause.
Who could achieve remission?
Some people with asthma are more likely to achieve clinical remission than others.
When appropriate treatments are started as soon as possible, and when the accumulative and irreversible lung damage from exacerbations can be minimised, the possibility of better outcomes for patients is improved. Timely intervention may also reduce their exposure to OCS and any of the associated side effects.
Emerging evidence now suggests that clinical remission could be possible for people with mild and moderate asthma, as well as those with severe asthma, by using the right treatment or combination of treatments at the right time. Severe asthma patients require a different combination of treatments to those with mild of moderate asthma. Taking medication in the correct way and continuing with treatment regimens also helps patients get the best outcomes.
“I do believe that there is a future within the next five years where we can start talking about really durable remissions in some patients with the disease and I think that’s going to be really amazing,” says Dr Chupp.
Is remission possible in other immune-mediated diseases?
Advances in science and medicine means that clinical remission is already considered an accepted treatment goal in many other immune-mediated conditions, such as rheumatoid arthritis and eosinophilic granulomatosis with polyangiitis (EGPA).
These conditions have a common link: a dysfunction in the immune system that gives rise to overactivity and excessive inflammation, causing it to attack the body as if it were a threat.
Identifying drugs that address the precise dysfunction in the immune system without dampening the entire system is a challenge scientists continue to explore.
“We are determined to redefine the future of respiratory medicine and achieve ambitious treatment goals for millions of people with asthma,” Katharina Wolff, Vice President of Global Medical Affairs at GSK, says.
“Our research into clinical remission in asthma could enable patients to achieve long-term freedom from exacerbations and the need for oral-corticosteroids, while also maintaining their lung function and providing optimal symptom control.
“This is just one example of how we are working to improve the daily lives of people with asthma and protect their future health.”